[ad_1]
Natural disasters such as earthquakes, tornados, and hurricanes are generally described in terms of wind speed, land area, and inches of rain. They’re also described in terms of human costs, such as the number of fatalities and injuries. Hurricane Katrina, for example, led to approximately 1,000 deaths in Louisiana, of which 75 percent were among adults age 60 or above.
What are the hidden health costs, though, that might not be reported immediately, but which are a result of a natural disaster? Some studies have looked at stress disorders, but a new study from researchers and scholars at Tufts University examined changes in the number of cardiovascular disease (CVD) hospitalizations before and after Katrina, and the disparate effect of Katrina on black and white older adults in Louisiana.
The co-first author on the study is Ninon Becquart, a former scholar in the NIH-funded Post-Baccalaureate Research Program (PREP) at Tufts who used R, SQL, and ArcMap to conduct sophisticated data analysis, including visualization. She was mentored on the research project by Elena Naumova, chair of the Division of Nutrition Data Science at the Friedman School of Nutrition Science and Policy at Tufts.
“Our goal with this research was to contribute to a methodology to assess the impact of natural disasters,” said Becquart. “We saw that rates spiked after Katrina’s landfall in all older adults, especially in older black adults. The rates appear to stabilize about two months after landfall, which coincides with the clearing of floodwaters from New Orleans.”
“We can expect to see more natural disasters because of climate change. Our study is one of the few that addresses the impact of natural disasters on CVD hospitalization rates, as well as disparities in hospitalization rates between black and white older adults,” said Naumova. “Considering the staggering social, economic, and health impacts of such disasters, we hope this study leads to more research and helps to inform emergency health preparedness.”
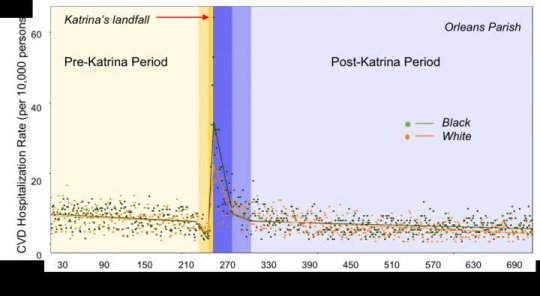
The research team focused on changes in the daily rates of cardiovascular hospitalizations (per 10,000) for adults aged 65 and older in three Louisiana parishes (counties), Orleans, Jefferson, and East Baton Rouge, over 710 days for the period from January 7, 2005 to December 17, 2006. They segmented the observation period to correspond to six time periods before, during, and after the arrival and departure of Katrina.
Using data from the Centers for Medicare and Medicaid Services, the team assembled a database with daily hospitalization rates for all CVD hospitalizations in the three parishes over the 710 days. They added U.S. Census data supplemented by American Community Survey estimates to obtain demographic and population measures.
Preliminary analysis included mapping the daily CVD rates across parishes and work with the data to identify the existing trend line for the CVD hospitalizations. They used the smoothed time series to define the six time segments and develop segmented linear regression models for the overall population in each parish and then separately for the black and the white populations.
CVD hospitalization rates had been stable or declining in each parish, but — in Orleans and Jefferson parishes — rose precipitously immediately after landfall. This increase in CVD hospitalization rates was prolonged, lasting more than a month after landfall. Notably, the increase in CVD rates was higher among the older black population compared to the older white population, after landfall, indicating differences in the level of impact in these two populations.
Over the study period, in East Baton Rouge Parish, CVD hospitalization rates were consistently higher on average for black adults, confirming what has been reported in the literature previously. No significant changes in CVD hospitalization rates were noted after landfall. The researchers speculate that this was because East Baton Rouge received more evacuees than parishes more directly hit by the hurricane, but also note that hospitals were overwhelmed and data might not be complete. In addition, they note that psychological stress has emerged as a risk factor for cardiovascular disease.
The 2017-18 hurricane seasons were particularly devastating, as storms like Harvey, Irma, Maria, and Jose ravaged major metropolitan hubs in Houston, Puerto Rico, and Dominica alongside the back-to-back disasters of Florence and Michael in Carolinas and Florida.
The NIH-funded PREP program at the Sackler School of Graduate Biomedical Sciences at Tufts is based on the idea that an enriched hands-on experience in research is the best preparation for additional training. It is designed to encourage students from under-represented groups to become research scientists. As a result of this project, and related coursework, Ninon has decided to focus on data analysis with the hopes of eventually completing a graduate degree in data science.
[ad_2]