[ad_1]
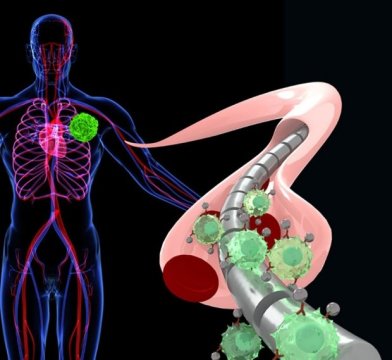
A magnetic wire used to snag scarce and hard-to-capture tumor cells could prove to be a swift and effective tactic for early cancer detection, according to a study by researchers at the Stanford University School of Medicine.
The wire, which is threaded into a vein, attracts special magnetic nanoparticles engineered to glom onto tumor cells that may be roaming the bloodstream if you have a tumor somewhere in your body. With these tumor cells essentially magnetized, the wire can lure the cells out of the free-flowing bloodstream using the same force that holds family photos to your refrigerator.
The technique, which has only been used in pigs so far, attracts from 10-80 times more tumor cells than current blood-based cancer-detection methods, making it a potent tool to catch the disease earlier. The technique could even help doctors evaluate a patient’s response to particular cancer treatments: If the therapy is working, tumor-cell levels in the blood should rise as the cells die and break away from the tumor, and then fall as the tumor shrinks.
For now, Sam Gambhir, MD, PhD, professor and chair of radiology and director of the Canary Center at Stanford for Cancer Early Detection, is focused on the wire as a cancer-detection method, but its reach could be much broader.
“It could be useful in any other disease in which there are cells or molecules of interest in the blood,” said Gambhir, who developed the wire with the help of his colleagues. “For example, let’s say you’re checking for a bacterial infection, circulating tumor DNA or rare cells that are responsible for inflammation in any of these scenarios, the wire and nanoparticles help to enrich the signal, and therefore detect the disease or infection.”
The study will be published online July 16 in Nature Biomedical Engineering. Gambhir is the senior author. Postdoctoral scholar Ophir Vermesh, MD, PhD; surgery resident Tianjia Jessie Ge, MD; and MD-PhD student Amin Aalipour share lead authorship.
No vial of blood necessary
Cells that have sloughed off the tumor and cruise the bloodstream freely, otherwise known as circulating tumor cells, can serve as cancer biomarkers, signaling the presence of the disease.
Why then, you might wonder, would you need an entirely new way to capture cells milling about the blood? Couldn’t a simple blood draw siphon off the same floating tumor cells? Hypothetically, yes, but circulating tumor cells are often scarce, and a blood draw only samples a few milliliters of the total blood volume, which in adult humans is about 5 liters.
“These circulating tumor cells are so few that if you just take a regular blood sample, those test tubes likely won’t even have a single circulating tumor cell in them,” said Gambhir, the Virginia and D.K. Ludwig Professor of Clinical Investigation in Cancer Research. It would be like searching for a grain of sand in a bathtub, but only scooping out a few cups of water.
“So doctors end up saying, ‘Okay, nothing’s there.'”
That, Gambhir said, is where he sees the magnetic wire making a difference. For the wire, which is about the length of your pinky finger and the thickness of a paperclip, to work, circulating tumor cells must be effectively magnetized with nanoparticles. The nanoparticles contain an antibody that latches onto circulating tumor cells. Once the floating tumor cell and nanoparticle are hitched, the cell lugs the tiny magnet around with it, and when the cell-magnet complex flows past the wire, it’s compelled by magnetic force to veer from its regular path in the bloodstream and stick to the wire. Then, the wire is removed from the vein, and the cells are stripped for analysis.
Gambhir and his team have yet to try out the wire in people, as they still have to file for approval from the Food and Drug Administration, but they have successfully tested it in pigs, placing the device in a vein near the pig’s ear. That vein is fairly similar to veins in the human arm. When compared with a 5-millileter blood sample, the magnetic wire extracted 10-80 times more cancerous cells; compared with a different, commercially available wire-based detection method, the wire picked up 500 to 5,000 more tumor cells.
“We estimate that it would take about 80 tubes of blood to match what the wire is able to sample in 20 minutes,” Gambhir said. Of course, he continued, it’s not practical to remove 80 test tubes of blood from one person; that’s more than a half-liter. “So, we’re hoping this approach will enrich our detection capability and give us better insight into just how rare these circulating tumor cells are, and how early on they exist once the cancer is present.”
A flexible wire
Gambhir said the technique could also be used to gather genetic information about tumors located in hard-to-biopsy places or to provide information about the efficacy of a cancer treatments. Perhaps most intriguingly, the magnetic wire may even stand to evolve into a treatment in and of itself.
“If we can get this thing to be really good at sucking up cancer cells, you might consider an application where you leave the wire in longer term,” Gambhir said. “That way it almost acts like a filter that grabs the cancer cells and prevents them from spreading to other parts of the body.”
Now, Gambhir is working to ready the technique for humans, which involves approval for the nanoparticles. His lab is conducting toxicity studies in mice, paying close attention to what happens to leftover nanoparticles that don’t bind. So far, there are no signs of toxicity, and the extras decay over the course of a few weeks, he said. Gambhir is also looking into nanoparticles that are already FDA-approved, working to tweak them for use with the wire. Once the technology is approved for humans, the goal is to develop it into a multi-pronged tool that will boost detection, diagnosis, treatment and evaluation of cancer therapy.
The work is an example of Stanford Medicine’s focus on precision health, the goal of which is to anticipate and prevent disease in the healthy and precisely diagnose and treat disease in the ill.
The study’s other Stanford authors are veterinary research coordinator Yamil Saenz, DVM; former graduate students Chin Chun Ooi, PhD, and Yue Guo, PhD; radiology and molecular imaging scientist Israt Alam, PhD; senior research scientist Seung-min Park, PhD; graduate student Charlie Adelson; postdoctoral scholars Hamed Arami, PhD, and Yoshiaki Mitsutake, PhD; assistant professor of comparative medicine Jose Vilches-Moure, DVM, PhD; life science technician Elias Godoy; research scientist Michael Bachmann, MD, ScD; preclinical laboratory managing director Jennifer Lyons; instructor of radiology Kerstin Mueller, PhD; life science technician Alfredo Green; Shan Wang, PhD, professor of materials science and engineering and of electrical engineering; and chemistry professor Edward Solomon, PhD, who is also a professor of photon science at SLAC National Accelerator Laboratory.
Gambhir is a member of Stanford Bio-X, the Stanford Cardiovascular Institute and the Stanford Neurosciences Institute.
The study was funded by National Institutes of Health (grants U54CA151459, R21CA185804 and S10 RR026714), the Canary Foundation and the Ben and Catherine Ivy Foundation.
[ad_2]