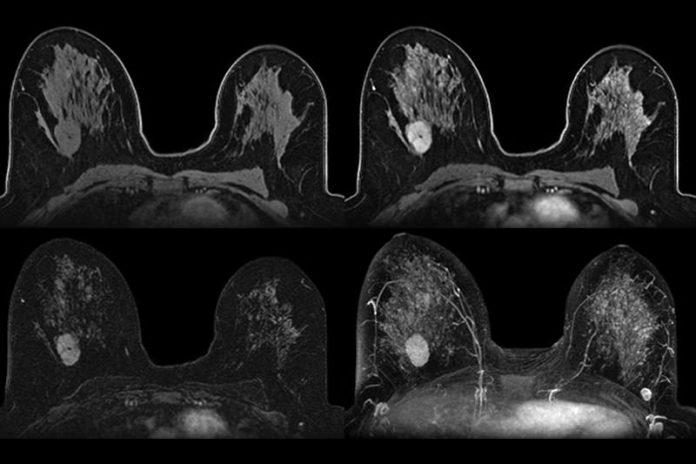
It has been estimated there will be 234,190 new cases of breast cancer in 2015 for both sexes and 40,730 estimated deaths. The goal of screening exams for breast cancer is to find cancers before they start to cause symptoms.
In a new study, a team of researchers from the Medical University of Vienna, Vienna, Austria; in cooperation with Memorial Sloan-Kettering Cancer Center, New York, had evaluated the breast cancer screening efficacy of mammography, ultrasound, and magnetic resonance imaging (MRI) in a high-risk population and in various population subgroups.
Dr. Thomas Helbich, MSc, MBA, Associate Professor of Radiology, University Clinic Vienna, Professor, Medical University of Vienna, Vice Chairman of the Department of Radiology, Medical University of Vienna, President, European Society of Breast Imaging along with Dr. Christopher Riedl MD, Department of Biomedical Imaging and Image-Guided Therapy, along with colleagues in a single-center, prospective, nonrandomized comparison study, BRCA mutation carriers and women with a high familial risk (over 20 percent lifetime risk) were offered screening with mammography, ultrasound, and MRI every 12 months. Diagnostic performance was compared between individual modalities and their combinations. Further comparisons were based on subpopulations dichotomized by screening rounds, mutation status, age, and breast density.
This study included 559 women with 1,365 complete imaging rounds.
The results showed the sensitivity of MRI was 90 percent significantly higher of all breast cancers clearly detected. Among the other modalities mammography detected 37.5 percent and ultrasound 37.5 percent. The combination of MRI and mammography increased the detection rate by just five per cent. None of the cancers were detected by ultrasound alone. The results were similar for non-invasive cancers and for benign breast lesions.
Of 40 cancers, 18 (45.0 percent) were detected by MRI alone. Two cancers were found by mammography alone (a ductal carcinoma in situ with microinvasion and a DCIS with less than 10- mm invasive areas. This did not lead to a significant increase of sensitivity compared with using MRI alone
Similarly, of 14 DCISs, all were detected by MRI, whereas mammography and ultrasound each detected five DCISs (35.7 percent). Age, mutation status, and breast density had no influence on the sensitivity of MRI and did not affect the superiority of MRI over mammography and ultrasound.
“In cases where there is even the slightest doubt, and especially in women at increased risk, the obvious choice is MRI. Our study clearly shows the superiority of magnetic resonance imaging over mammography and breast ultrasound examinations,” said Dr. Helbich. “The superiority of MRI is also completely independent of the patient’s age, gene mutation status and breast density.”
“An MRI scan carried out once a year is therefore the only alternative for high-risk patients who have a strong family history of breast cancer to the surgical removal of the breast and ovaries,” says Dr.Helbich. “This is by no means ‘over-diagnosis’, but rather a necessity. Around 13,000 women in Austria are still at increased risk of breast cancer.”
The results of the study, says the MedUni Vienna expert, should encourage the increased use of MRI for breast screening too. Says Helbich: “In light of these results, it is our duty to make women more aware of the fact that the use of mammography and ultrasound cannot detect all types of cancer. MRI really is the method to be recommended.”
Currently Austria has 15 MRI scanners per million inhabitants — putting the country above the EU average (10 scanners / million inhabitants). If MRI is to be used more frequently, Italian or Greek ratios would be better: in these countries, there are 24 and 23 MRI scanners per million inhabitants respectively.